On the road again….
Just can’t wait to get on the road again…::warbles::
Anyway – had a great time with friends, but I am driving home today. It’s about a 4 hour drive. I have another week before classes start, which is good since I have a lot to do to prepare! Once classes start it is going to be crazy, so I want to make sure my house is clean, my computer is organized, my syllabi/binders are in order, my pantries are stocked, etc. And most importantly, I want to get a chance to see my friends and hang out with them some, since I won’t get to see my non-OT friends very often after next week. The craziness is nearing, aughhhhhhhhhhhhhhh!
It should be an exciting semester! It was great to have the month of June off to recover and steel myself for the upcoming onslaught!
Lessons come to life: observations in the NICU and SCU
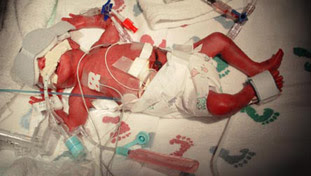
Intraventricular hemorrhage (IVH), Necrotizing Enterocolitis (NEC), Retinopathy of PRematurity (ROP), Gastroesophageal reflux (GER), Bronchopulmonary dysplasia (BPD)…and lions and tigers and bears.
When our “Perspectives of Early Development” professor had us fill out a worksheet on common diagnoses seen in the neonatal ICU in preparation for a visit there, I was only mildly interested. I thought it was a little cool to read about all the crazy things that happen to preemies, but wasn’t overly excited about things like “bronchopulmonary dysplasia”. It was just medical terminology, just another thing to remember.
Then I did my first Level I fieldwork in a pediatric hospital. And all my learning suddenly came to life. Because it seemed like every single kid in the NICU and SCU had a spectrum of respiratory, cardiac, neurological, and gastrointestinal problems. (Duh, that’s why they are there!!!) They all seemed to have G-tubes or NG tubes, nasal cannulaes, ostomy bags, you name it. It was shocking to realize that in the two weeks I was there, I probably only saw a child feed by mouth once or twice. Their charts were filled with abbreviations like BPD, IVH Stage III, NEC, ROP…they all struggled to breathe and threw up constantly. The lucky ones had Nissens (although I recently read a really interesting post on why Nissens aren’t that great of an idea somewhere in Ryntales.blogspot.com, who is a mother who spent like half a year in the NICU with her baby). ANYWAY, I learned all about things like looking for conjugate gaze, bilateral reaching, flexion, muscle tone, oxygen saturation levels, and more. It was so fascinating. All the beeping monitors and the babies protruding tubes were a little bit overwhelming at first, but with a great OT at the helm showing me the ropes, it all became a little bit more normal and a little less alien. Those kids need all the OT they can get!
—
I’m still out of town but plan to be back late Saturday. School starts back a week into July, so I’ll have some new material to discuss pretty soon!
OTs put the FUN in functional
Hey readers (all like, six of you), I’ll be in a travelling flux until Wednesday, so don’t expect anything new for a few days. I leave you with this to check out if you are bored:
www. cafepress.com has some great OT t-shirts. Just search for “occupational therapy” there or along those lines and see what pops up. My two favorites say something like:
“OTs put the fun in functional”
“OT makes Every Day Independence Day”
You can also create your own OT t-shirt there!
The t-shirt posted is just a random one I found on google images, though. 🙂
A Snail's Pace: Patience is a Virtue

It’s hard to sit on my hands. Whether I am helping a kid, a peer, or my grandma, I have a difficult time being patient. I like to be efficient, and when I watch someone do something slowly, it makes my skin crawl. In everyday life, it often doesn’t matter who does the task, and frequently it is easier for everyone if the fastest person does it. In rehabilitation, it’s a different story.
I bet that most OT’s have had to sit on their hands constantly. OTs are usually efficient multi-taskers, and the USA has a fast-faced society, chronologically bound. With insurance time-limits and overscheduling, there isn’t always the luxury of waiting for a patient to finish a task on their own time. Just in my limited years of observation, I’ve often watched in admiration as the OT does patiently watch and not help while a patient slowly completes some activity. I feel like yes, some OTs are naturally more patient than others, but that it is probably mostly a learned skill, cultivated from days, months, years of practice in a rehab setting.
At several points during the semester, our class has been able to observe people with various issues who were subsequently very slow to handle ADLs like grooming, dressing, cooking, etc. There has been several times where I have been in pure and utter agony while watching someone complete a task s l o w l y, because I wanted to help so badly . I know I am not the only one who felt that way, because I would watch some of the other students fidget or held their hands clasped behind their back, as if they knew their hands would flutter to help if left free. After a few minutes of watching these tasks, I always just want to scream ENOUGH ALREADY PLEASE LET ME HELP YOU FOR THE LOVE OF ALL THAT IS GOOD IN THIS WORLD!!!!!!!! Luckily, the screams stay in my head.
Now, I realize the whole point is for the client to be independent, and that it certainly isn’t easy with a bunch of people watching, and that it is amazing the clients have the patience to keep trying without any visible frustration. So it is not that I don’t understand or realize the point of these exercises (usually to show us how assistive devices work or alternate ways to do something). They are great learning experiences and very helpful for a variety of reasons. But more than anything else, they are HUGE reminders to me that I need to work (a lot) on the virtue of patience.
I will have to sit on my hands quite a bit in the beginning, and slowly cull the experience needed to help me figure out when the patient has reached their frustration overload and I should intervene, versus when I should sit there serenely, benignly encouraging and verbally cuing the patient, hands OFF!
*Disclaimer: as always, all names, details, situation changed – only the moral lesson remains the same.
Don't judge a book by its cover
This is another lesson I learned while on my first fieldwork in a pediatric hospital a few months ago, which I found while looking through my journal. Absolutely all aspects of the situation have been changed for confidentiality reason, but the lesson remains the same. Fake details included only because it makes it more interesting!
————
Our next patience was a young boy accompanied by his parents. At first glance, they appeared very out of place in a hospital setting. *They were covered in tattoos and piercings, with brightly dyed hair and ripped clothing with inappropriate slogans.* OR: *They were an older couple, clearly recent immigrants that didn’t speak much English* OR: *They were a younger couple, dressed as if they had been out all night clubbing* They appeared ill-at-ease and tense. I steeled myself to observe rude, uncaring parents.
As the OTs started talking to the parents, I realized immediately how wrong I had been in my initial assessment. They were caring and kind and clearly cared very much about their child. They spoke in broken language spattered with grammatical errors, but what mattered is that their words were filled with love. The parents pointed out some of the problems their child was having, and the OTs talked with them about the issues needing intervention versus those that might be outgrown on their own. It was a good visit and it was clear the couple would do whatever necessary for their beloved child.
It may not sound like rocket science to realize you shouldn’t judge a book by its cover, but it was really an eye-opening moment for me. I realized appearances are not always as they seem. An individual can be well-dressed and well-educated and be a horrible parent, while an oddly-dressed or odd-looking individual might be an amazing parent. It was a good lesson to learn early.
—————
Update: Merrolee (New Zealand educator, blog on sidebar) and I exchanged several e-mails about this post. Originally, I just focused on the couple looking odd. But we discussed (ok, she explained and I listened/agreed) that this post isn’t really just about appearance. It could be the language, the demeanor, the interaction type, the skin color, the language, the cultural norms…anything that would potentially cause an OT to make a snap judgment about that person. The lesson is still the same – we must suspend judgment and realize that person might have a lot to offer that we don’t realize due to our (erroneous) first-glance assumptions of their capabilities. In my case, the original lesson I learned from this experience was that appearance isn’t always what it seems. With Merrolee’s guidance the lesson has dug in a little deeper to include all first impressions, whether it is cultural, social, or physical. She pointed out some interesting issues regarding confidentiality as well as cultural differences due to New Zealand’s diverse background, so hopefully she’ll consider writing a post about that! (Hint Hint)
Typical feeding session
I have been able to attend several feeding sessions during my first semester of OT school. I kept a very detailed journal of these sessions, although obviously I can’t share it in that form since it would violate HIPAA. I’ve therefore modified all the details about the session in this post, so that the information about the specific children is left out and only the treatment approach remains. Names changed too.
Sometimes feeding sessions are needed in OT or SLP due to a child having a host of oral issues including hyper or hyposensitivity and possibly sensory defensiveness. The OT I was observing, Connie, told me that she has had some children cover their eyes in panic when watching her eat something they find repugnant, such as pancakes due to their mushy quality. The sessions I watched were co-treats with a great SLP. Connie had me set up with washcloths, soapy water, and several large towels. I was inwardly thinking huh? Then the SLP came in with a ton of food from the cafeteria – turkey, green beans, cheerios, Doritos, pudding, goldfish crackers, etc. We were operating off this feeding workshop called
Apparently, the same procedure is used pretty much every time in order to accustom the child to the routine. The food varies slightly based on the child’s particular needs, but follows specific rules set by the SOS program, such as making sure each subsequent food shared a trait with the previous food. Of course that’s a simplified explanation. Anyway, here is how a typical feeding session would go, using this SOS program.
–
We started by all sitting at a table with the soapy basin. We each received a washcloth and had to dip the washcloth in the soapy water, squeeze it out, and wash our hands with it. Then put our washcloth behind our chair. The wet washclothes were present in case a child feels the need to wipe their face or hands, when dealing with foods that bother them.Then get a dry one to wipe off, and do the same. I was primarily there as a social modeler, ie doing whatever everyone else did, to show the child its normal, natural, give some mild peer pressure, etc. Connie then brought out some chocolate pudding and put a spoonful of it on all of our plates (sometimes the child is encouraged to pass out the food so that the child can feel in control). We then discussed its texture, its color, dipped it in our fingers, painted with it, licked it, experimented with it on our face, etc. We then moved on to another brown food, cheerios. We dropped these to hear the sound they made, discussed how they were crunchy, made patterns in the pudding, discussed color and shape. We then moved on to French fries, which are also brown. We discussed their long shape, pretending they were earrings, eyebrows, walking them around, discussing how soft they were, how we could tear them apart, how we could take a bite and move it around on our tongue, hide it in our mouth, spit it out…then we got out ketchup for the fries.
After the French fries I believe we moved on to another round object – green beans. At some point we moved onto goldfish crackers, which were popular. (I think I forgot a food or two in this since you wouldn’t go from green beans to goldfish crackers.) We discussed crunchiness, color, and so on. Then it was time for Doritos which are also orange, and triangles. Again, crunchiness was discussed. Now it was time to bring out another triangle – TURKEY MEAT. The OT pushed this into triangles and gave it to us and we ended up having to eat the Dorito and turkey meat together! The OT, Connie, gagged when she ate the Dorito-turkey but hid it well. I wanted to laugh.
Throughout this entire experience, we all had to smile, act enthusiastic, chew with our mouths wide open, make exaggerated swallows, chomps, show the food in our mouth, show our tongue and talk animatedly about how we use our STRONG TEETH, how the food goes into our mouth and into our TUMMIES, etc, etc.
At clean-up time, OT Connie and the child have to “blow” their food into the trash can. I was REALLY glad I did not have to do this part. They essentially have to bite into every food on their plate, and then spit it out into the trashcan. Many children balk at this since it involves having things in their mouth they don’t like. However, since the point is for enjoyment and not aversion, they aren’t pushed overly hard with this. Overall it has been fascinating to watch feeding sessions. I really enjoyed the learning experience!
=====
This is a picture of my favorite picnic sandwich while in CA – french bread, mortadella, brie, and chips. Yum. So eating a Turkey-Dorito in feeding group didn’t make me gag because it’s YUMMY!
There's no "I" in TEAM…groupwork.

I’m the tiniest bit bummed that if my blog address does get put in OT Practice (it might not!), people will be finding it while I am on my mini summer break. I don’t start back in school again until early July, so I don’t necessarily have a lot to talk about that is truly OT-student related for the next few weeks.
We haven’t gotten our grades yet, which I am waiting eagerly for, but we are starting to get new syllabi posted on “Blackboard”. In one of our upcoming classes we will be taking wood-working, and we also need to find a ceramics class and a leather-working class on our own time. We also have about ten bazillion group projects. I’ll admit it, I find group projects tedious and frustrating. But I also know they are good for us, and that as an OT in Rehab, we are pretty much ALWAYS going to be involved in teams, so I guess we need the practice in working together.
When y’all were in school, did you have to do a ton of group projects? Or as educators now, do you assign a lot of group projects? What are your thoughts on it?
When I am in a group project with one other person who carries their weight, I can understand the value of a group project, because the work can kind of be cut in half. But once there are more than two people, and especially if there are four or five, I start to lose my understanding of the value, because it seems like everything gets inefficient. Perhaps I just need to learn better group skills. Maybe that’s the point of all this group work.
OT Practice & Blogging
A few months back in AOTA’s OT Practice there was an article on blogging, Second Life, and podcasting, by Dr. Fran Babiss. It was really interesting and reminded me of how hard it had been to find any OT blogs at all, especially by OT students. Reading that article motivated me to start this blog that same day. I also wrote in to OT Practice that same inspired day to share my new blog address. There is a chance they will publish the address in the next OT Practice, since they were compiling a bunch of responses to the article to put in a forum. At the time I wrote in, I did not know of a single OT blog. Now of course I know about the few students (Patti, Aishel, Aishah), Merrolee’s amazing group, and a few other solitary OT bloggers like Will Wade (all linked on my sidebar). I’m glad we have a core group, but I sincerely hope that we’ll get some new bloggers soon! I especially personally have an interest in seeing more blogs by practicing clinicians and students.
We’ll see if the address gets published (we’d know before the end of June) and if so, hopefully it will have a domino effect where we will all get a few more readers!!
Mental Health: Autobiography Poem
To me, the poem below describes exactly what OTs try to teach their patients when working in the mental health field.
AUTOBIOGRAPHY IN FIVE SHORT CHAPTERS
by Portia Nelson
I
I walk down the street.
There is a deep hole in the sidewalk
I fall in.
I am lost … I am helpless.
It isn’t my fault.
It takes me forever to find a way out.
II
I walk down the same street.
There is a deep hole in the sidewalk.
I pretend I don’t see it.
I fall in again.
I can’t believe I am in the same place
but, it isn’t my fault.
It still takes a long time to get out.
III
I walk down the same street.
There is a deep hole in the sidewalk.
I see it is there.
I still fall in … it’s a habit.
my eyes are open
I know where I am.
It is my fault.
I get out immediately.
IV
I walk down the same street.
There is a deep hole in the sidewalk.
I walk around it.
V
I walk down another street.
==========================================
PS: I took this picture in my house. A bazillion mental dollars to anyone who can figure out what it is. Hint: It’s not a neuron. But it kinda looks like one, so it’s a wonderfully subtle (until now) picture for a mental health post!!
Hallmark OT Appreciation Cards
Do you ever get thank you cards from patients? It’s not like you can go to Hallmark and buy special OT Appreciation cards.
But if I worked for Hallmark these are the kind of cards I would make:
I like to sing and I like to dance… and thanks to my OT I can don and doff my pants.
I can only move against gravity,
I guess that gives me a muscle strength of three.
But here’s my OT walking through the door,
soon I’ll have a muscle strength of four!!
Thanks to OT I can get to the loo..even if it is a max assist x 2.
I don’t need any whistles or bells…
thanks to OT I can complete my ADLs.
PS: This is a picture of the snail-dessert we made my grandfather for Father’s Day, while visiting him in Berkeley. It involves a madeleine cookie, whipped cream, berries, and butterfinger crumbles. Assembled on a colored cutting board. My sister and I were quite proud of our creativity.

